The material is for informational purposes only and does not replace an in-person consultation.
Most often the conversation begins with one short phrase: “I have noticed a small lump near my navel”.
A person usually does not come with a ready diagnosis. They come with an observation. “Sometimes it is visible, sometimes not”. “After physical effort it protrudes more”. “If I lie down – it seems to go away”. At this point it is important not so much to name the condition as to understand it correctly. Because a protrusion in the umbilical area is not always the same thing. And even when it is indeed a hernia, hernias behave differently: in some people it remains small for years, while in others it noticeably progresses within several months.
As a surgeon, I look at the situation through three questions that the patient usually does not formulate aloud, but they are exactly what determines the management strategy: what exactly is protruding, why it appeared now, and whether there are signs that the problem is no longer “just a protrusion” and is moving into a risk zone. When these three answers are clear, anxiety disappears. What remains is a plan of action.
How an umbilical hernia usually begins
An umbilical hernia rarely starts as an acute event. More often it begins as a small, almost everyday finding. This is where the trap lies: if it does not hurt, it must not be dangerous. In practice, the absence of pain usually only means that there are no complications yet. But the defect in the abdominal wall may already have formed.
What patients notice first
The most common sign is a protrusion in the umbilical area that becomes more noticeable when the abdomen is strained. Some people notice it in the mirror after a shower, some accidentally feel it with their fingers, and others notice a change in the shape of the navel: it seems to “turn outward”.
There are typical details that repeat from case to case. In a woman after childbirth it often looks like this: several months after pregnancy she returns to her usual activities, resumes physical effort, and suddenly notices that the navel looks “different”. The protrusion is small, soft, sometimes disappears. There is almost no pain, at most a feeling of tension by the end of the day. In such situations many people attribute everything to diastasis or “postpartum recovery” and postpone consultation.
In a man with physical work the story has a different rhythm. He may say: “I lifted something heavy and in the evening noticed a bulge”. There does not have to be a single traumatic effort. Sometimes it is the result of regularly increased intra-abdominal pressure: lifting, straining, coughing in a smoker. At first the protrusion is small, “like a pea”, and then becomes more noticeable.
An athlete has his own scenario. Most often it is strength training or functional exercises where there is powerful core tension. He usually feels his body well and notices changes faster: “After an abdominal workout or after deadlifts I felt pressure around the navel”. And here it is especially important not to fall into false reassurance, because physical fitness does not protect against tissue defects. It only masks the problem until the defect becomes significant.
Why the protrusion may appear and disappear
The mechanics of this phenomenon are simple, but they often mislead people. Inside the abdominal cavity there is pressure. It increases when a person coughs, laughs, lifts something heavy, strains during constipation, performs a strength effort, or sharply tightens the abdominal muscles. If there is a weak point in the umbilical area, tissues begin to move outward through the defect. This creates the protrusion.
When a person lies down and relaxes the abdomen, the pressure decreases. The contents of the protrusion may partially or completely return back, and outwardly it seems that “everything has gone away”. But it is not the cause that disappears – only the manifestation. The defect in the abdominal wall remains.
This “variability” of symptoms is one of the important diagnostic signs. It helps distinguish a hernia from some other conditions, and helps the patient understand why the situation can seem stable for years and then suddenly begin to change.
What actually happens in the umbilical area
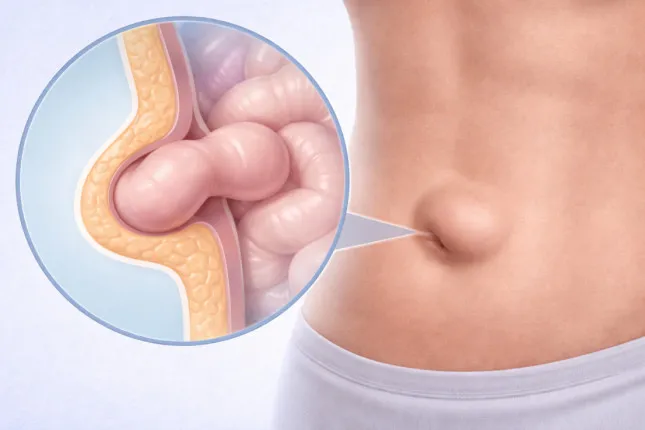
To stop fearing the unknown, it helps to imagine what exactly changes in the tissues. An umbilical hernia is not a “lump”, not inflammation and not a tumor. It is an architectural problem of the abdominal wall: an opening appears there through which internal structures begin to protrude.
How a defect of the abdominal wall forms
The anterior abdominal wall is not just “abdominal muscles”. It is a multilayer framework: muscles, fasciae, and tendinous sheaths. It must hold the organs in place and withstand pressure from within. If part of this framework becomes weaker, it begins to stretch. At first this is barely noticeable. Then a defect forms – the very “opening” through which tissues begin to protrude under the skin.
In the early stages, preperitoneal fat tissue most often protrudes. That is why a small hernia may be soft, painless, and easily reducible. Later other structures may enter the hernia sac, and that is when observation and proper risk assessment become especially important.
Why the navel is a natural weak point
The navel is a special anatomical area. It is the place where the structures of the umbilical cord passed during fetal development. After birth the umbilical ring closes, but the tissue in this region is initially different from the surrounding areas. It is thinner and more prone to stretching.
Therefore, when conditions arise for constant or repeated increases in intra-abdominal pressure, the navel naturally becomes one of the “exit points”. Not because the body has “failed”, but because that is how the anatomy is designed.
Who most often encounters an umbilical hernia
In surgical practice there are recognizable patient profiles. Not because everyone is the same, but because the mechanics of the disease repeat themselves. What matters is the combination of load and the quality of connective tissue. In one person the tissues withstand serious loads for years. In another the defect appears against relatively everyday factors. This is not the patient’s “fault”, but rather the characteristics of the tissues combined with circumstances.
Typical patients in surgical practice
A woman after pregnancy. The classic moment is several months or a year after childbirth. The protrusion is small and usually painless. A woman may notice that it increases when lifting a child, during abdominal exercises, or with constipation. Often there is also diastasis nearby, and everything is perceived as one “postpartum story”, although the management of diastasis and a hernia differs fundamentally.
A man with physical work. Usually this is someone whose workload is regular while recovery and prevention are absent. He may not notice a small hernia for a long time until it begins to interfere with work or becomes painful. A common detail is a chronic cough or a habit of straining, which constantly increases intra-abdominal pressure.
A patient with excess weight. Here it is not only the number on the scale that matters, but the constant load on the abdominal wall. In such patients a hernia may progress faster because the pressure acts daily. Concomitant conditions are often present as well, increasing the risk of complications and influencing the choice of management.
Patients after surgery. After interventions on the abdominal wall the distribution of load changes, scars form, and areas of tissue become less elastic. Not every protrusion after surgery is a hernia, but the overall risk of hernia defects is higher. That is why in this group it is especially important not to guess but to confirm the diagnosis clinically.
These profiles are not included merely for “the beauty of the text”. They help the reader recognize themselves and understand that their story is typical and therefore predictable. For the physician they help quickly assess probabilities and risks without missing important nuances.
How to distinguish an umbilical hernia from other conditions
Perhaps the most useful skill for a patient is to understand that not every protrusion in the abdominal area is a hernia. But the opposite mistake is also dangerous – attributing a hernia to “weak abs” or “postpartum changes” and doing nothing for years.
How a hernia differs from diastasis
Diastasis is a separation of the rectus abdominis muscles along the midline, most often after pregnancy or due to connective tissue changes. In diastasis there is no “hole” in the abdominal wall in the same sense as in a hernia. Instead there is widening of the linea alba, which leads to a longitudinal protrusion along the center of the abdomen during tension, sometimes appearing like a “ridge”.
An umbilical hernia is a local defect, most often in the area of the umbilical ring. The protrusion is more rounded and localized. It may be reducible and may appear during coughing. And most importantly, with a hernia there is a risk of incarceration. With diastasis this risk usually does not exist.
Sometimes diastasis and a hernia coexist. In such cases management is determined not only by aesthetics and comfort but also by safety.
When a protrusion may not be a hernia
Sometimes a bulge in the umbilical area is visible due to subcutaneous fat tissue, anatomical features of the navel, scar changes after piercing, or inflammatory processes. In some cases patients describe a “lump”, but during examination it turns out that this is not a hernia but another local formation of the skin or subcutaneous tissue.
The key principle here is simple: a diagnosis is made not from photographs and not from sensations, but from a clinical examination. The doctor checks whether there is a defect, whether the protrusion changes with tension, whether it can be reduced, and which tissues are involved. This takes minutes but can save months of anxiety and experiments.
Why a hernia may not bother for a long time
An umbilical hernia often remains quiet. And it is precisely this quietness that makes it deceptive. A patient may think: “If I am used to it, it must be safe”. But in surgery what matters is not habit but prognosis.
Why many patients postpone visiting a doctor for years
The reasons are usually very human. No pain – no motivation. There is work, children, responsibilities. Plus there is fear of the word “operation” and the expectation that the doctor will insist on immediate surgery. Because of this people choose observation without diagnosis, and these are different things. Observation means the diagnosis is confirmed and the risks are assessed. Delayed consultation means a person simply hopes that “it will not get worse”.
Patients whose hernia is reducible and barely noticeable postpone consultation especially often. They literally do not see the problem every day. But a hernia follows its own rules, not a person’s schedule.
What happens to a hernia over time
The defect in the abdominal wall rarely becomes smaller. More often it slowly expands. The volume of the hernia sac increases, its contents change, and the probability of painful episodes rises. At the same time a person may develop factors that increase intra-abdominal pressure: weight gain, coughing, constipation, reduced physical activity with loss of muscle tone. As a result the “small lump” that had been just a peculiarity for years gradually becomes a symptom.
There is also another scenario well known to surgeons: a large hernia that did not cause pain for a long time suddenly produces an acute episode. The patient says: “I have had it for a long time, but it never bothered me”. And this very “never” makes the episode particularly unexpected.
When the situation becomes dangerous
The danger of an umbilical hernia is related not so much to the size of the protrusion as to the risk of incarceration. Incarceration is a situation when the contents of the hernia become trapped in the defect and the tissues cannot return back. At that moment the problem stops being cosmetic and becomes urgent.
How hernia incarceration develops
Imagine a ring through which tissues pass. If the tissues exit and become fixed, the outflow of blood is disturbed. First pain appears. Then swelling develops, which further increases compression. It becomes a vicious circle. In such a situation it is important not to wait “until it passes”, but to act quickly. Time here is a medical factor, not a figure of speech.
Patients sometimes try to force the hernia back themselves. This is a bad idea, especially if the pain is significant. A doctor evaluates the situation carefully: what exactly is trapped, how pronounced the signs of impaired blood supply are, and whether there are associated intestinal symptoms. Self-manipulation may worsen tissue damage.
Symptoms that require urgent medical attention
There are signs that should be considered a reason for urgent medical care:
– sudden or increasing pain in the area of the navel and protrusion
– the protrusion becomes firm, painful, and no longer reducible
– redness of the skin and local warmth in the area of the protrusion
– nausea, vomiting, pronounced weakness
– absence of stool or gas, abdominal bloating
Not all these symptoms must appear at the same time. Sometimes it begins with one sign, but early reaction reduces the risk of severe consequences.
Can an umbilical hernia be treated without surgery
The question of surgery is always emotional. Therefore it should be framed correctly. The issue is not whether it is possible “to endure”. The question is whether a defect of the abdominal wall can be closed without surgical repair. And here the answer is clear: in adults a formed defect does not close on its own.
Why exercises and support belts do not close the defect
Exercises strengthen the muscles, improve core control, help posture and load management. This is useful. But exercises cannot “sew up” an opening in the aponeurosis. If a defect exists, it remains.
A support belt may temporarily reduce the protrusion and relieve discomfort during effort, and in some situations it may be used as supportive management. But a belt is not treatment. It does not eliminate the cause – it only mechanically supports the area. As soon as the support disappears, the manifestations return.
An important detail: long-term “treatment with a support belt” sometimes creates a false sense of control and postpones the moment when the problem could be solved in a planned and calm manner.
What happens if a hernia is simply observed
Observation is possible, but it should be a conscious decision after examination by a surgeon. The doctor considers the size of the defect, reducibility, symptoms, lifestyle, comorbidities, and the risk of complications. After that, the management strategy is chosen. Sometimes it is indeed reasonable to plan intervention not urgently but at a convenient time. Sometimes it is wiser not to delay because the prognosis of progression is unfavorable.
The most dangerous situation is not observation itself but the absence of diagnosis and risk assessment. This is the zone where patients most often lose time.
How a surgeon confirms the diagnosis
Diagnosis of an umbilical hernia in most cases does not require complex investigations. But it does require a proper examination. Details matter: how the protrusion behaves with tension, whether there is a defect, how reducible it is, whether there is tenderness, and which tissues are involved.
Examination and clinical diagnosis
The examination usually includes assessment in standing and lying positions, a test with slight tension of the abdominal wall, and palpation of the umbilical ring area. The doctor does not simply “look”. They check whether there is a hernia gate, its size, whether there are signs of adhesions, and how freely the contents move.
For an experienced surgeon, a clinical picture is already formed at this stage: what type of defect it is, how stable it is, what the risk of complications is, and which questions need further clarification.
When ultrasound is needed
Ultrasound is useful when it is necessary to clarify the contents of the hernia sac, the size of the defect, the characteristics of the tissues, or when the clinical picture is not obvious. Ultrasound also helps differentiate a hernia from other local formations in the umbilical area.
It is important to understand: ultrasound does not replace examination by a surgeon. It complements it when truly necessary.
How an umbilical hernia is treated today
This section should be perceived as guidance rather than an “instruction”. The choice of treatment method depends on the size of the defect, the condition of the tissues, associated factors, and the patient’s lifestyle. One principle is essential: the goal of treatment is to restore the strength of the abdominal wall and reduce the risk of recurrence and complications.
The general principle of surgery
The essence of the intervention is to eliminate the hernia defect and strengthen the area of the umbilical ring. This can be done in different ways. The option is selected individually because the same method is not equally suitable for different patients. An athlete with a small hernia and a patient with excess weight and a large defect have different initial conditions, and this influences the decision.
Importantly, modern approaches allow treatment to be planned so that the patient understands the stages of preparation, the recovery timeline, and the limitations. This reduces anxiety and increases predictability of the outcome.
When mesh is used
A mesh implant is used when the patient’s own tissues cannot provide reliable closure of the defect or when the risk of recurrence without reinforcement is too high. The decision depends on the size of the hernia gate and the quality of the tissues. The purpose of the mesh is not to “replace the muscles” but to reinforce the defect area and distribute the load so that the abdominal wall functions stably.
At the same time, mesh is not “always mandatory”. In some situations, options without it are possible. However, the choice is made not according to the patient’s wish “I want no mesh” but according to the assessment of the risk of hernia recurrence.
How recovery takes place
Recovery usually includes limiting heavy physical effort for a certain period, gradual return to activity, and following recommendations regarding daily routine. It is important not only to “get through the first days” but to allow the tissues to heal properly. It is during this period that the long-term strength of the result is formed.
In real clinical practice the best recovery is seen in patients who perceive rehabilitation not as a prohibition but as a stage of treatment. They do not glorify early physical effort and do not test the repair “as a challenge”. This is not about weakness – it is about medical awareness.
Myths That Cause Patients to Delay Treatment
Umbilical hernia is surrounded by myths because outwardly it often appears “not serious”. Because of this, a person may live with the defect for years without understanding the risks. Clarifying these myths is useful not to frighten patients, but to bring clarity to the situation.
A Hernia Can Go Away on Its Own
In adults, a formed umbilical hernia does not close spontaneously. It may temporarily decrease when lying down or when physical load is reduced, but this is not healing – it is simply a change in manifestations. The tissue defect remains.
If It Does Not Hurt – It Is Not Dangerous
Pain is not the main criterion. The absence of pain usually only means that there are no complications at the moment. The risk of incarceration depends on the anatomy of the defect and its behavior, not on subjective comfort. That is why it is more reasonable to evaluate a hernia electively rather than when the situation forces urgent action.
Hernia Surgery Is Always Difficult
Fear of surgery is often associated with other people’s experiences and with the era of “old surgery”. Modern approaches have significantly changed patient experience and the predictability of recovery. More importantly, elective treatment is almost always calmer and safer than intervention performed in the presence of complications. That is why discussion about treatment is best done in advance, when there is time and choice.
What Is Important to Understand About Umbilical Hernia
An umbilical hernia is a well-understood and predictable surgical condition. It begins with a small sign that is easy to underestimate. But its development follows certain patterns: tissue defects rarely disappear on their own, and the risk of complications exists even when symptoms are minimal.
The most reasonable step for a person who notices a protrusion near the navel is to confirm the diagnosis with a surgeon and evaluate the risks. This does not mean deciding “surgery today”. It means clarity. And clarity in medicine almost always reduces anxiety more effectively than promises that “it will go away on its own”.
There is also another principle that often becomes key for patients: treating a hernia electively means managing the situation. Treating it in the presence of complications means trying to catch up with the situation. In clinical practice the difference between these two scenarios is very clear.
Clinical Guidelines and Sources
- Henriksen NA, Montgomery A, Kaufmann R, et al. Guidelines for treatment of umbilical and epigastric hernias from the European Hernia Society and Americas Hernia Society. British Journal of Surgery. 2020
- HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018
- De Simone B, Birindelli A, Sartelli M, et al. Emergency repair of complicated abdominal wall hernias: WSES guidelines. World Journal of Emergency Surgery. 2020
- World Society of Emergency Surgery (WSES). Emergency repair of complicated abdominal wall hernias – consensus conference recommendations. 2013
- American College of Surgeons (ACS). Adult Umbilical Hernia. Patient Education
- Brunicardi FC, Andersen DK, Billiar TR, et al. Schwartz’s Principles of Surgery. McGraw-Hill
- Townsend CM, Beauchamp RD, Evers BM, Mattox KL. Sabiston Textbook of Surgery. Elsevier.
- Kulaçoğlu H. Current options in umbilical hernia repair in adult patients. 2015
- StatPearls (NCBI Bookshelf). Umbilical Hernia. Continuously updated review

